
Body Composition, Nutrition and COVID
Lifestyle Factors and Health
Body Composition, Nutrition and COVID
Patricia “Trish” Sheean, PhD
Dr. Sheean: I have expertise in retrospective cohorts, which is going back in the medical record and designing studies so that you can answer questions to address different components of causality.
So COVID-19 really represented an unbelievable opportunity to look at body composition in an unprecedented group of people in the ICU.
People were coming in with COVID-19 and going into the ICU. In the beginning, they were getting a lot of chest CTs and abdominal CTs, and that’s where we were able to leverage a rich archive of body composition data. It was a great opportunity to look at body composition by race and ethnicity - something unexplored in acutely ill patients until now. Maybe there was something going on that could explain these different outcomes by race and ethnicity because we know in healthy populations, our body composition actually does differ by race and ethnicity. Perhaps there was something unique in this ICU setting, and in previous attempts we’ve never had the ability to do this. If you think about it, everybody’s coming in with the same diagnosis. They’re all getting a CT. It was so uniform and clean in design, and a fantastic opportunity to explore.
Talar Markossian, PhD
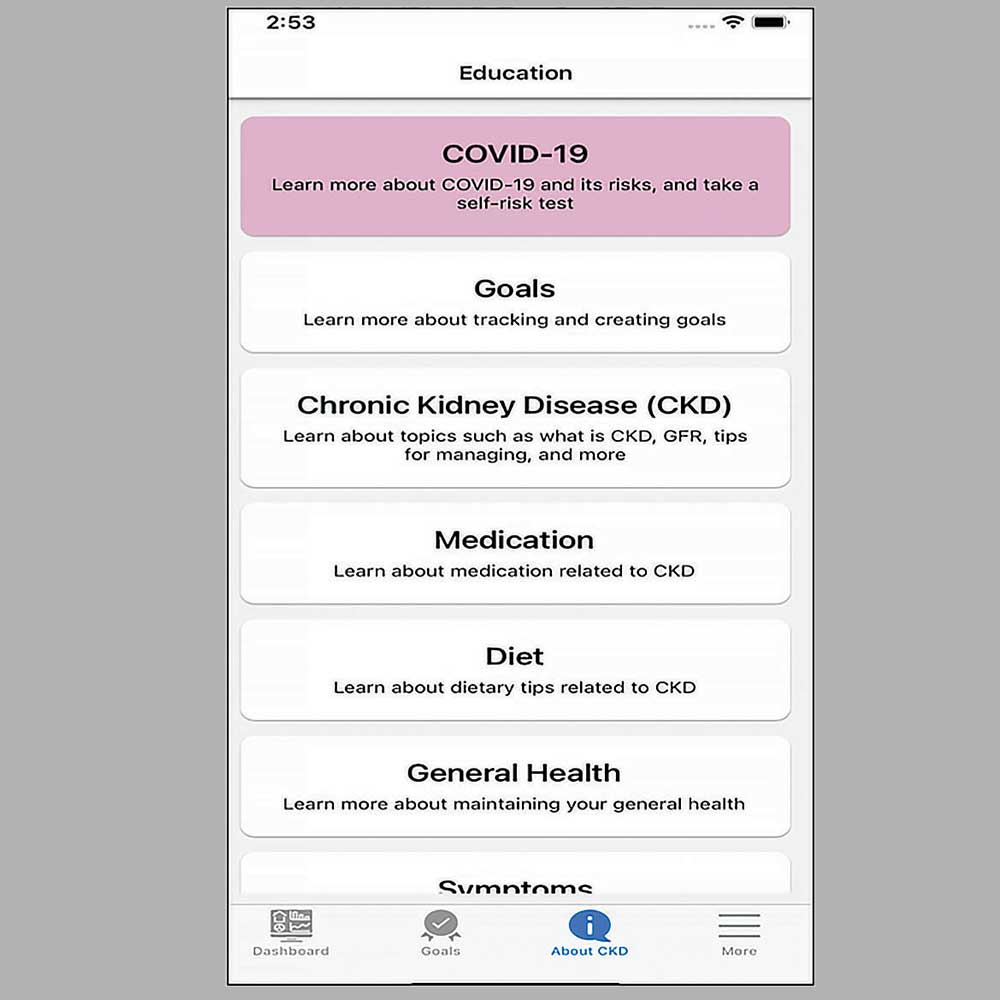
Chronic Kidney Disease Mobile App
Disease and Clinical Syndrome Prevention
App supports CKD self-management and patient communication
Learn More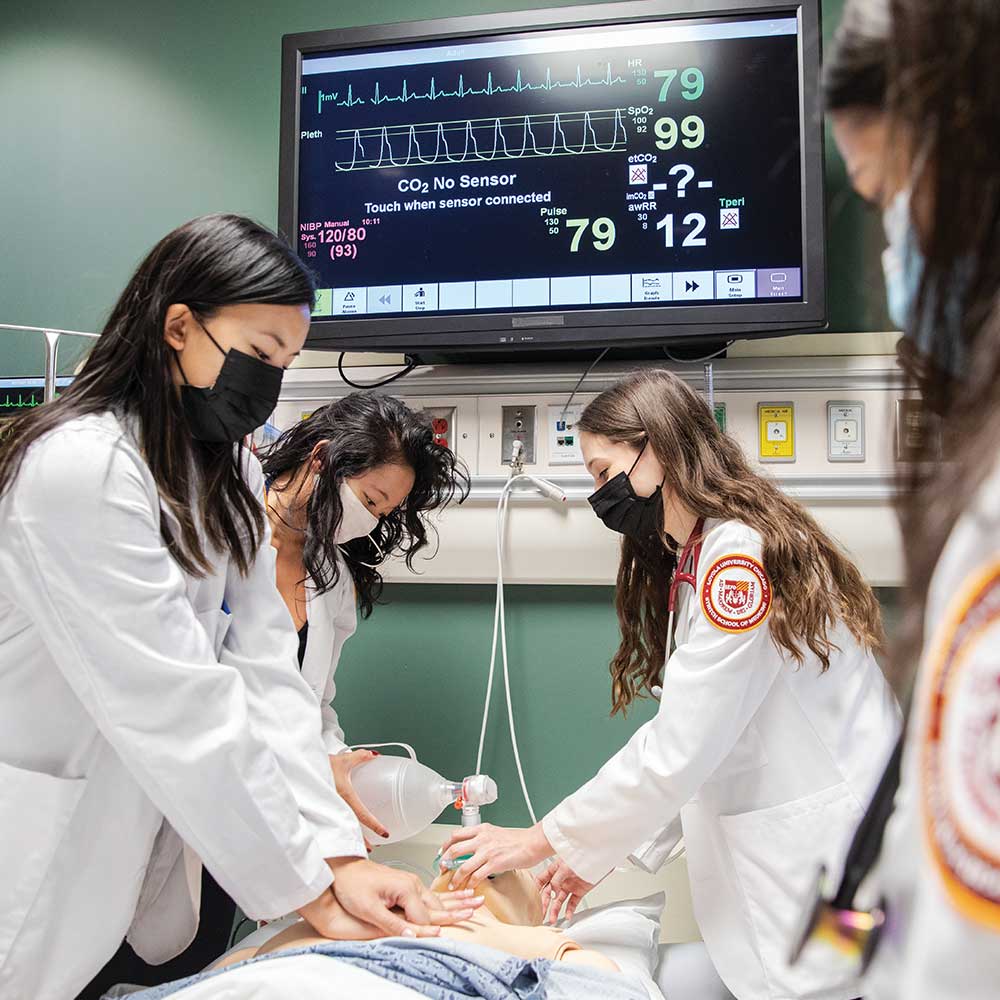
Mohammad Samie Tootooni, PhD
Respiratory Distress and Heart Health
Disease and Clinical Syndrome Prevention
AI-driven cardiopulmonary prediction and data integration
Learn More
Idiake “Dee” Irumundomon
Idiake “Dee” Irumundomon
Loyola Stands Against Gun Violence Summit
Empowering students through advocacy and community engagement
Learn MoreAnd this was a sample size of about 200 patients?
There were a lot of people coming in with COVID-19, but they had to have a particular kind of CT and then we had to be able to actually retrieve it. So all of those factors made it a little bit harder to get to our target number. We ended up with 141 patients.
What conclusions did you arrive at?
We published a paper looking at body composition and outcomes. We spent months and months refining the methods and approach. We collected a lot of data trying to look at the implications between body composition, COVID-19 and nutrition support. Remember, I am a clinical dietitian. I come at it thinking everybody who comes in the ICU is theoretically supposed to be getting some kind of nutrition GRANT PROFILES support, right? If a patient is intubated, cannot breathe or therefore eat on their own, we need to feed them using a tube.
The national guidelines advise providing 25 calories per kilo. So we thought feeding would have big implications on outcomes in this population. What we found, what was really novel, was that how sick a patient was at the time of admission was more important than anything else. It had nothing to do with the color of their skin, body composition differences or other factors. It was really driven by how sick the patient was at the door.
We used something called an APACHE score to look at how sick patients were. An APACHE score uses a complicated matrix of clinical values at ICU admission to predict outcomes. So in other words, APACHE was a better predictor than body composition, malnutrition, and many other factors. No one had looked at this through this lens using the statistical techniques and team approach we had. We published this paper and have a few other papers in the pipeline.
Patricia “Trish” Sheean, PhD
Dr. Sheean: I have expertise in retrospective cohorts, which is going back in the medical record and designing studies so that you can answer questions to address different components of causality.
So COVID-19 really represented an unbelievable opportunity to look at body composition in an unprecedented group of people in the ICU.
People were coming in with COVID-19 and going into the ICU. In the beginning, they were getting a lot of chest CTs and abdominal CTs, and that’s where we were able to leverage a rich archive of body composition data. It was a great opportunity to look at body composition by race and ethnicity - something unexplored in acutely ill patients until now. Maybe there was something going on that could explain these different outcomes by race and ethnicity because we know in healthy populations, our body composition actually does differ by race and ethnicity. Perhaps there was something unique in this ICU setting, and in previous attempts we’ve never had the ability to do this. If you think about it, everybody’s coming in with the same diagnosis. They’re all getting a CT. It was so uniform and clean in design, and a fantastic opportunity to explore.
And this was a sample size of about 200 patients?
There were a lot of people coming in with COVID-19, but they had to have a particular kind of CT and then we had to be able to actually retrieve it. So all of those factors made it a little bit harder to get to our target number. We ended up with 141 patients.
What conclusions did you arrive at?
We published a paper looking at body composition and outcomes. We spent months and months refining the methods and approach. We collected a lot of data trying to look at the implications between body composition, COVID-19 and nutrition support. Remember, I am a clinical dietitian. I come at it thinking everybody who comes in the ICU is theoretically supposed to be getting some kind of nutrition GRANT PROFILES support, right? If a patient is intubated, cannot breathe or therefore eat on their own, we need to feed them using a tube.
The national guidelines advise providing 25 calories per kilo. So we thought feeding would have big implications on outcomes in this population. What we found, what was really novel, was that how sick a patient was at the time of admission was more important than anything else. It had nothing to do with the color of their skin, body composition differences or other factors. It was really driven by how sick the patient was at the door.
We used something called an APACHE score to look at how sick patients were. An APACHE score uses a complicated matrix of clinical values at ICU admission to predict outcomes. So in other words, APACHE was a better predictor than body composition, malnutrition, and many other factors. No one had looked at this through this lens using the statistical techniques and team approach we had. We published this paper and have a few other papers in the pipeline.
